Blog
Helpful resources on environmental allergies, food allergens, and more
What It Actually Takes to Launch Allergy Services in 90 Days
Congratulations, you have made the decision to add a new service to improve your patients’ and your practice’s health—allergy testing and immunotherapy. Now what? Adding allergy testing and immunotherapy sounds complex, but it’s not with the right partner and mindset. Of course, there are the…
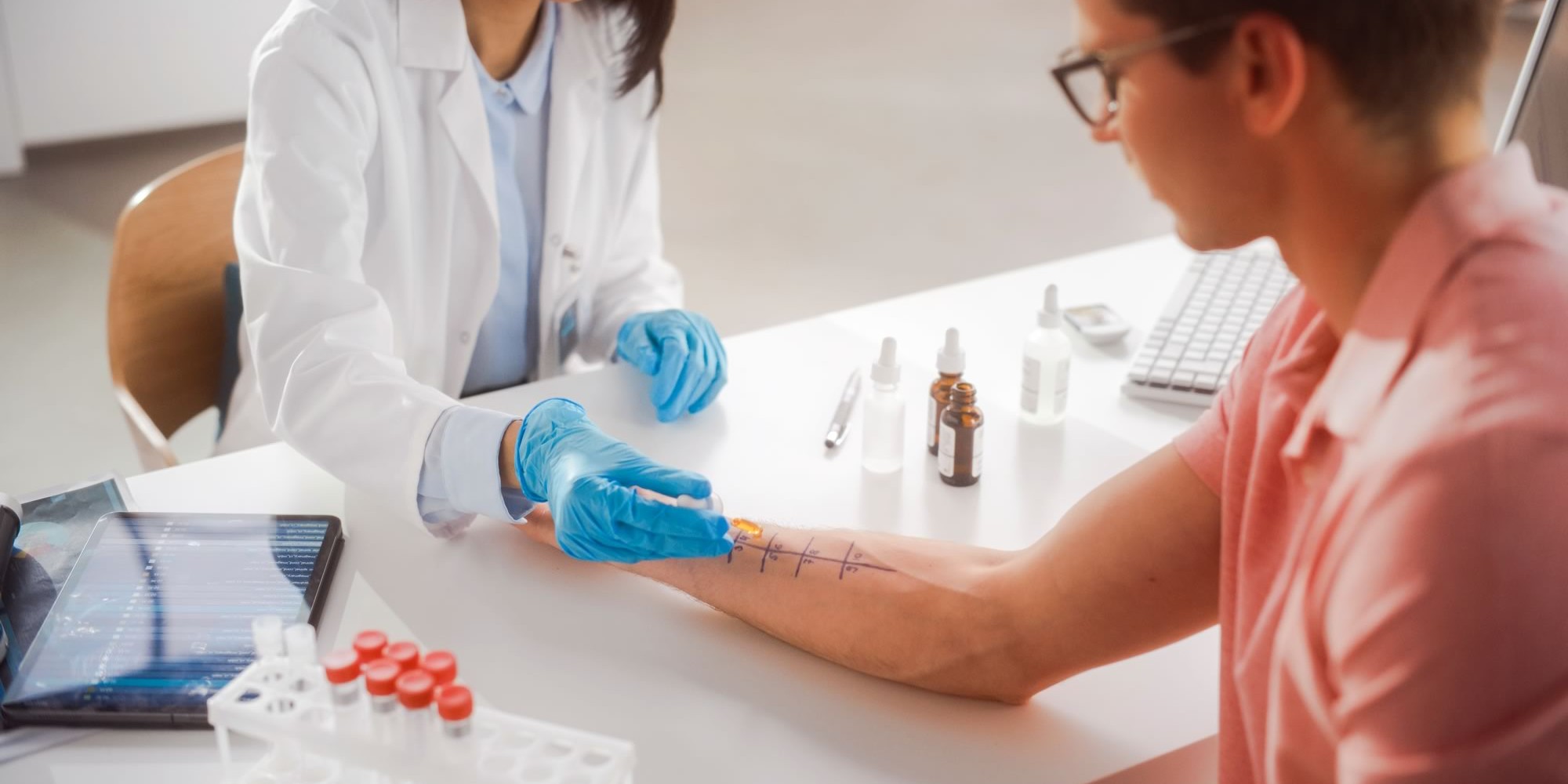
Is Your Practice Ready for Spring Allergy Season?
Every spring, there is a surge of patients experiencing symptoms such as congestion, sinus pressure, itchy eyes, cough, fatigue, and headaches. While these allergy symptoms are common, seasonal allergies affect more than 100 million Americans each year, making allergic rhinitis one of the most…
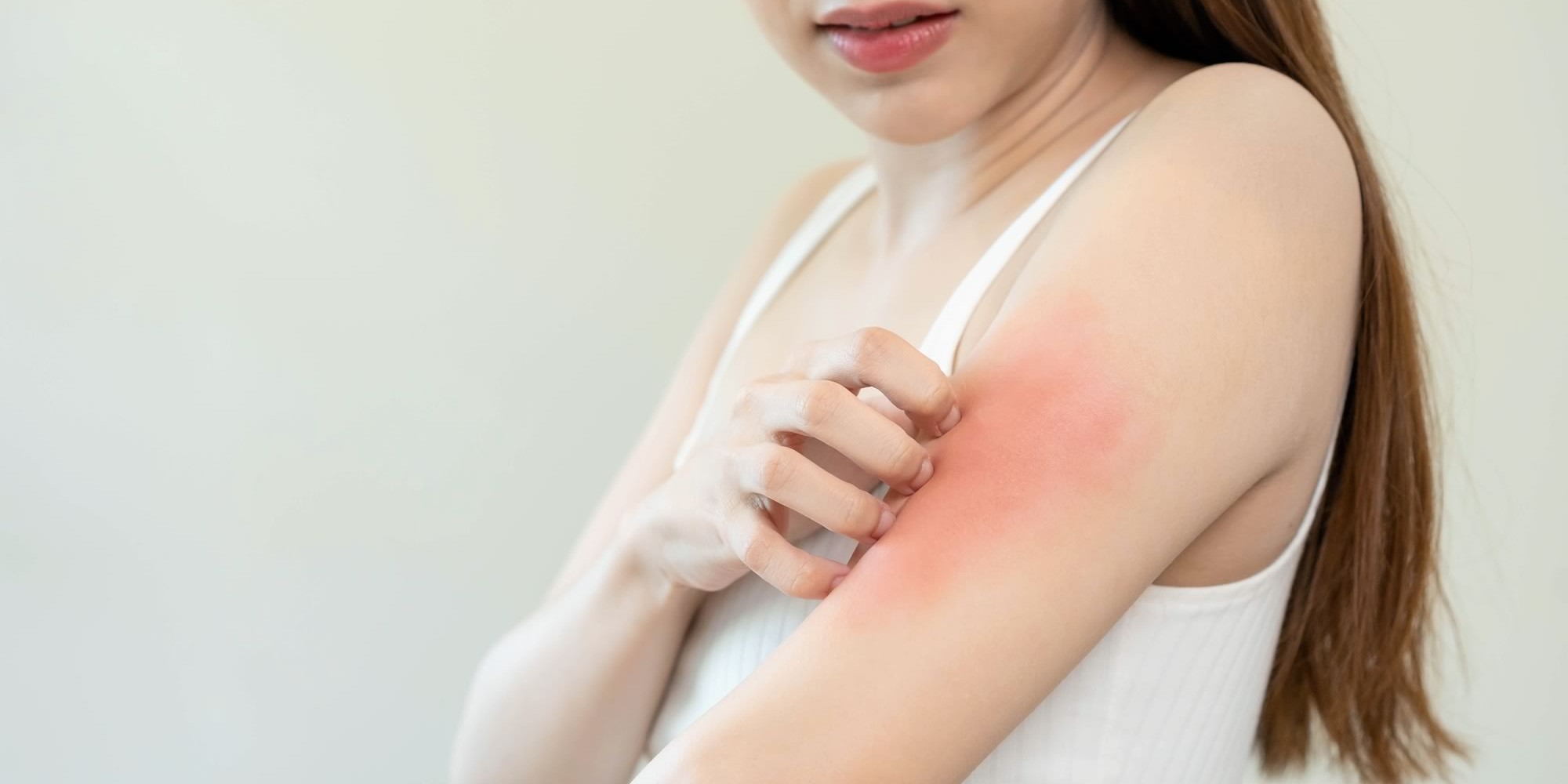
USP <797> Explained: What Physicians Need to Know When Preparing Allergen Immunotherapy In-Office
As regulatory standards evolve, many physician practices are asking an important question: How does USP <797> impact the way we prepare allergen immunotherapy (AIT) in our office? Whether you are currently mixing allergy extracts on site or considering adding immunotherapy services to your…
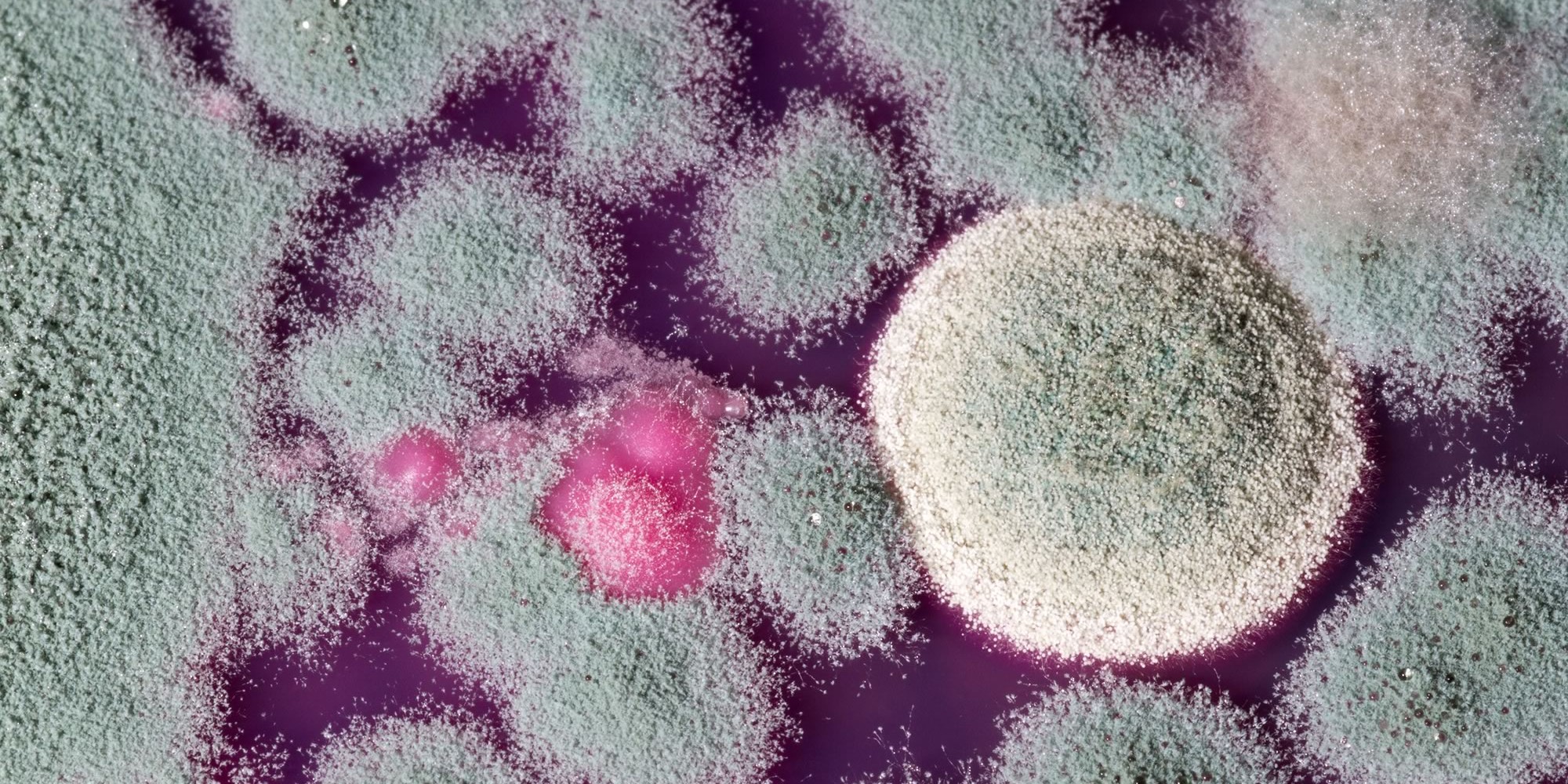
Cold, Flu, or Allergies? How to Tell the Difference this Fall
Not sure if your symptoms are from a cold, the flu, or allergies? Learn how to tell the difference and when to see a provider. Take the Allergy Quiz or Find a Provider near you today. Understanding the Confusion Every fall, countless people wonder: Is it a cold, the flu, or allergies? Each…
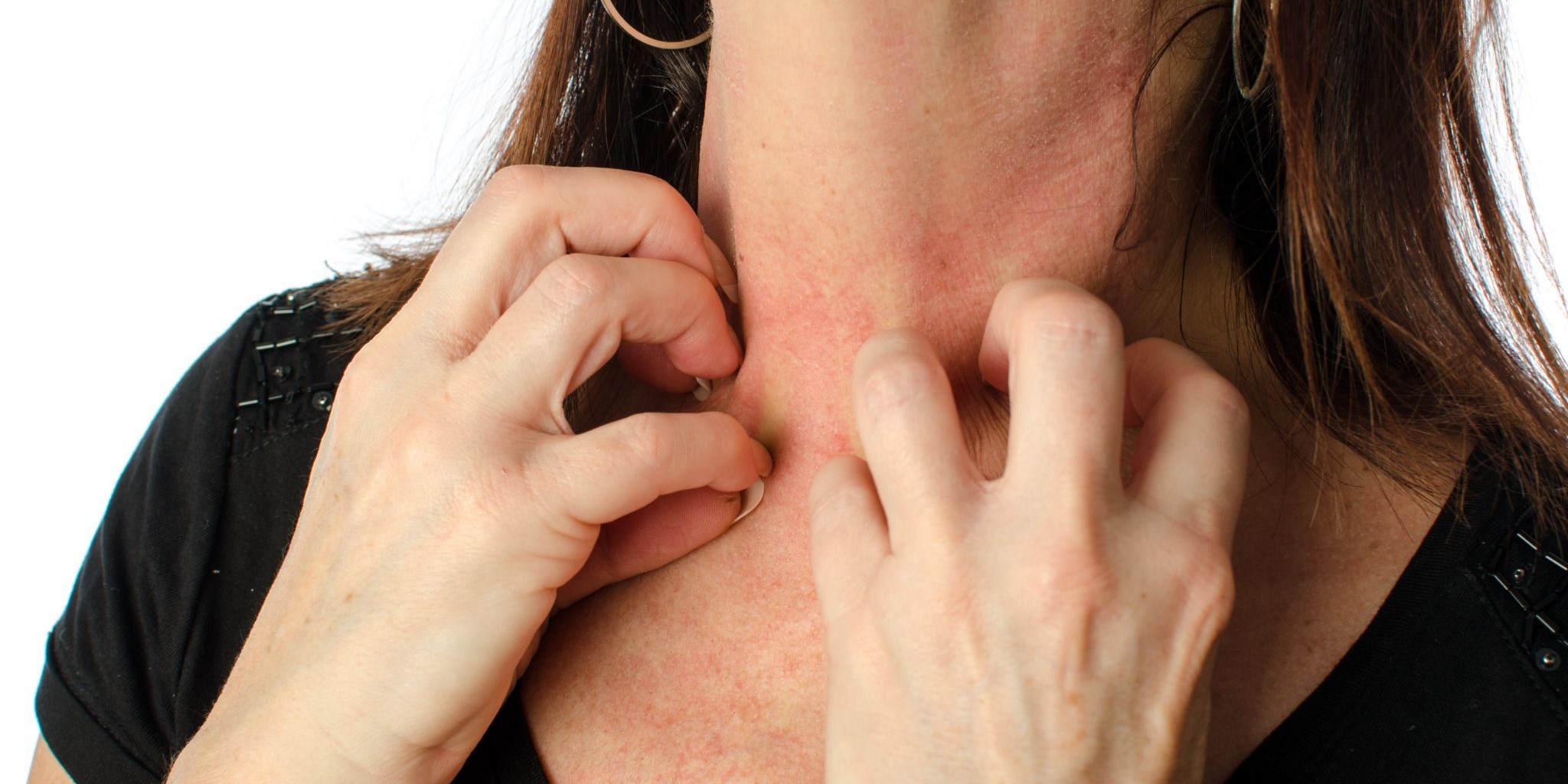
Rising Ragweed Pollen: Why Fall Allergies in the U.S. Are Getting Worse
Every fall, ragweed pollen has long been a familiar culprit behind sneezing, congestion, and itchy eyes. But lately, it’s not just the symptoms that are changing—it’s the season itself. Rising ragweed pollen levels are making allergy season longer, more intense, and harder to escape. What…
Fall Allergy Relief: How Provider Practices Can Lead the Way
As summer starts to give way to fall, and the first cool front arrives, many patients brace for seasonal allergies. While ragweed often steals the spotlight, fall allergy sufferers face a broader spectrum of triggers—from varied pollen sources to mold and dust mites. For many providers, this season…
Allergy Services for Primary Care Physicians: Expanding Access to Long-Term Allergy Relief
Allergies affect more than 100 million people each year. Yet despite their widespread impact, allergies often go untreated due to the scarcity of specialist care. That’s why United Allergy Services is focused on introducing allergy treatment and immunotherapy to primary care practices—the first and…
United Allergy Services Featured in Fujitsu Case Study
We are happy to share that United Allergy Services was recently featured in a Fujitsu case study highlighting how we achieve precise inventory tracking and process automation to enhance patient safety and efficiency. The case study explores how UAS leverages Fujitsu’s GLOVIA® OM solution, in…
Allergy Testing Kits & Immunotherapy from UAS: A Flexible Solution
Adding allergy care allows healthcare providers to address a common patient need and create a new income stream within the existing framework of their practice. However, we know that every medical practice has different requirements. For practitioners looking to integrate allergy testing and…
Pediatrics: How Early Allergy Testing & Treatment Can Benefit Young Patients
Allergies are a common yet often overlooked concern in pediatric care, affecting millions of children across the U.S. While allergy symptoms like sneezing, itchy eyes, and congestion may seem minor, untreated allergies can lead to more serious conditions, including asthma, chronic sinus infections,…
The Primary Care Practice Crisis: It’s Time to Play Offense
In an article published in Medical Economics, Brad J. Scoggins, FO, DAAP contends that it’s not enough for medical practices to counter adverse market forces by cutting costs and streamlining operations. He argues that practices must take steps to generate more revenue—specifically by offering…
Case Study: Adding Allergy Testing and Immunotherapy to Patient Care
A thriving practice delivering comprehensive patient services in-house, including family care, pediatrics, internal medicine, rheumatology, gynecology, and dietitian services, wanted to expand its offerings with on-site allergy testing and immunotherapy. The practice’s physician team strived to…
Maximizing Your Practice by Minimizing the Leakage
Does your medical practice have leaks? Is your growth hindered by “lost business” that negates the full impact of new patient growth? One of my favorite business expressions is from Roger Enrico, the former CEO of PepsiCo, who would say: “Growth is what matters.” It was one of the cornerstones that…
Why Offer Allergy Treatment for Children?
For providers passionate about providing care to the pediatric population, integrating fundamental allergy care into their practice can bring about significant benefits. Allergy screening, testing, and treatment fosters healthier lives and also enhances the overall quality of care that can be…
How Does UAS Partner with Providers?
How can healthcare providers balance the demands for more patient quality time and the financial requirements for a sustainable practice? Although it may seem counterintuitive to offer an additional service line, doing so can deliver higher revenue, additional clinical support, and meet rising…
Why Offer Allergy Care Services in Your Medical Practice?
More than 100 million Americans suffer from environmental, seasonal and perennial allergies, including ragweed, pollen, dust mites and animal dander. In addition, roughly 11% of adults and 7½% of children have a food allergy. Unfortunately, only a fraction seek treatment from a specialist,…
Ancillary Medical Services
In today’s world of declining insurance reimbursements and a multitude of competing options for patients to access care, vibrant, healthy practices are constantly seeking opportunities to grow. Growth can come from expanding your patient base as well as expanding your offerings by offering…
Am I Suffering from Allergies? Or Something Else?
There is a wide range of variability from person to person when it comes to allergies. The unique circumstances of each person and their environment as well as what type of symptoms occur, how often they occur, and how troublesome they are all have significant meaning. Gathering this…
A Deep Dive into Summertime Allergies
As the warmth of summer graces us with its presence, many of us are eager to embrace outdoor activities and soak up the sun. However, along with the barbecues, beach days, and sunny strolls, comes an uninvited guest: allergies. For many people, summer is synonymous with sniffling, sneezing, itchy…
FSA/HSA Plans for Allergy Services
Environmental allergies are a common ailment that affects approximately 50 million Americans every year. Whether you suffer from year round or just seasonal allergies, you may be able to use your tax-free FSA/HSA funds to help you save money on education, allergy testing, and treatments. If you…
Oral Allergy Syndrome
Delicious, ripe, mouthwatering fruits and vegetables are more plentiful during these summer months. However, that that summer breeze may carry more than just excitement for the season. Some people with environmental allergies may notice that certain fruits, vegetables, or nuts give them distinct…
Summer Allergies
What do you look forward to in the summer months? I bet it isn't summer allergies! Whether you are planning to be the grill master or the ultimate host of the patio celebration, we have tips to help you prepare. Today, let’s discuss some common summer allergens you may encounter when enjoying the…
Eosinophilic Esophagitis (EoE)
Eosinophilic esophagitis (EoE) is a recognized diagnosis that produces symptoms related to dysfunction of the esophagus. In EoE, large amounts of white blood cells, specifically eosinophils, collect in the inner lining of the esophagus resulting in inflammation. Typically, the esophagus is free…
Allergies, Asthma, and Air Quality
As we move into the summer months, it is important to understand the connection between allergies, asthma, and air quality. While air pollution does not directly cause allergy or asthma, it can increase the risk of developing atopic disease. Air pollution can also trigger allergy or asthma symptoms…
Earth Day and Climate Change Effects
Earth Day is this Friday, April 22nd. Earth Day is truly a mainstay in American culture, created by Past-President Richard Nixon. This year the Earth Day theme is “Invest in Our Planet”. We are called upon to have “unstoppable courage to preserve and protect our health, our families, our…
Easter and Passover Allergy Concerns
The Easter and Passover holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, holidays like Easter and Passover can be challenging to navigate with traditional holiday foods containing hidden allergies, and the high…
Botanical Sexism: Does it impact allergy sufferers?
What is Botanical Sexism? Tom Ogren, horticulturist and allergy researcher, has done extensive research on ways to reduce pollen counts and pollen potency. His theory centers around the unbalanced planting of male vs female plants. This unbalance can impact pollen counts and the resulting…
Tree Pollen and Pollen Counts Explained
March is here, and so is Spring! Spring has officially started which brings longer days, refreshing rain showers, bright colorful flowers, and of course…tree pollen! The majority of trees typically produce tree pollen as early as January in the Southern United States. The Northern and Central areas…
St. Patrick’s Day, Green Beer, and Wheat Allergy
St. Patrick's Day is fast approaching! Are you wondering if your wheat allergy will get in the way? History of the Holiday In Ireland, the holiday was created as a way to honor the country's patron saint and a time to cut loose during the Catholic Lent season. Today, the holiday is honored in…
Shake off the winter blues!
Winter blues setting in? Dreaming of springtime? Well, the wait is almost over! March is a week away, and that means Spring is on its way! Longer days, long walks in the garden, and rain showers and rainbows are on the horizon. The meteorological calendar says spring begins March 1st, but the…
Six More Weeks of Winter
The first official Groundhog Day celebration took place on February 2, 1887, in Punxsutawney, Pennsylvania, and was the brainchild of local newspaper editor Clymer Freas. He sold a group of businessmen and groundhog hunters on the idea of gathering around the inaugural famous groundhog to see…
The BIG 9: Food Allergens
For the last 17 years, the official list of major food allergens, or “The Big 8” has consisted of milk, egg, fish, shellfish, peanut, tree nut, wheat, and soy. The Big 8 were part of legislation that was signed into law in 2004 requiring manufacturers to indicate on labels when a product was made…
Prepare for Spring Allergy Season
Spring is fast approaching, and if you are a seasonal allergy sufferer, you likely associate this time of year with chronic sneezing, sniffling, and coughing. Your immune system is armed and ready to defend against harmless pollens, sending histamine soaring in your body triggering sneezing, runny…
Contraindications for Immunotherapy
Allergies are not always clear cut and simple to understand. A person may assume that a certain food or substance is the cause of their allergy symptoms and relate it to allergies, or they may not see the complete picture. We know allergy testing is extremely beneficial in allowing a provider to…
2022 – New Year, New You!
Happy New Year, and welcome 2022! The start of a new year arrives for many with guilt-laden resolutions to improve things like personal health goals. Resolutions to improve health can seem overwhelming and cause anxiety if they are unrealistic in the end goal or timeframe. Allergy and asthma…
Helpful Hints for the Holidays
The holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, holidays like Christmas, Hanukkah, and Kwanza can be challenging. First, traditional holiday foods containing hidden allergies may be present. Also at risk is…
Eczema and Atopic Dermatitis
We have made it to the highly anticipated holiday season! We ate more than our share of turkey, taken down the last of the fall décor, have started trimming the tree, and are double down on the holiday gift lists. With winter weather upon us or in the near future, and personal care products a…
Dust Mite Allergy
Halloween may be over, but there are certain creepy creatures that diligently remain year-round and commonly trigger allergy and asthma symptoms. Dust mites are eight-legged relatives ticks and spiders, have no eyes, have translucent bodies, and are microscopic, or too small to see with the unaided…
Respiratory Care Week, October 24-30
As we settle into this final week of October and prepare for some frightful fun at the end of the week, let’s all take a big deep breath in before the end of the year holiday season is upon us! Speaking of that big deep breath, October is Healthy Lung Month and this week, October 24-30 is…
Football, Food, and Fall Allergies
Fall has arrived and so have shorter days, cooler weather, and football season! Unfortunately for some, football, food and fall allergies go hand in hand. This is especially true in the southern and western regions of the US where some weed allergens peak in the fall. The idea of sneezing and…
Flu, Allergies, Cold, or COVID?
With the approaching fall season, we typically witness flu and viral season quickly arrive as well. Simultaneously weed pollen, dust mite, and mold allergy sufferers are preparing for an intense time of year. This year however, the ongoing spread of COVID-19 and reputable variants adds an…
Ragweed and Fall Pollen Allergies
Back to school season is here! Shorter days, crisp, cool evenings, and beautiful fall foliage are on the horizon. This time also marks the onset of weed pollination and the resurgence of allergy symptoms that may have taken a vacation in the hot, dry July heat. The meteorological calendar says…
Back to School Action Plan for Allergies and Asthma
As the final days of summer break come to a close, families everywhere are preparing for children to return to school. Whether this is the first year a child is heading to school or the last, it is an exciting time for both children and parents. It can, however, also be a time of anxiety for a…
Stinging Insects & Allergic Reactions
As summer continues marching on, the calendar surely includes upcoming cook-outs, boating on the lake or just a few hours playing in the backyard. The warmer temperatures and longer days present increased opportunities for visits for not so welcome winged visitors. While stinging insects may only…
Summer Allergy Travel Tips
School is out, summer is in full swing, and it is prime time for summer vacations and traveling. Summer travel with environmental allergies, asthma, or food allergies may make planning a vacation seem like a daunting task. Not to worry! We can show how to keep summer allergy issues at bay during…
Grass Pollen Allergy: Making the Most of Summer
Summer is finally here! Longer days, days spent by the beach or the pool, and late nights catching fireflies are on the horizon. Allergies are usually associated with the spring or fall because pollen is most active during these times. However, summer allergies, especially to grass, are also…
Independence from Summer Allergies
The Fourth of July is only one week away and that likely means many are making or finalizing plans to be outside. Are you planning to be the grill master? How about the fireworks expert? Maybe you are the ultimate host of the celebration surrounded by family and friends enjoying fireworks, picnics,…
Easter with Allergies
The Easter and Passover holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, they can sometimes be challenging to navigate. Aside from the usual pollen and food allergies, brightly dyed eggs, household pets, and sweet…
Tips for Balancing Baseball and Allergies
Spring means longer days, warmer weather, and the beginnings of baseball! Unfortunately for some allergy sufferers, the start of the long-anticipated baseball season also means the time of year when allergens such as tree pollen are at an all-time high. Sneezing, wheezing, and itchy, watery eyes…
Tips for Traveling with Allergies
Summer is here, and for many families that means a much anticipated vacation! A time for overdue rest and relaxation, or maybe some quality time spent away with children and loved ones. While fun can be had at its best during this time, allergies can be at their worst, leaving sufferers to fear…
Cold, Flu, or Allergies? How to Tell the Difference this Fall
Not sure if your symptoms are from a cold, the flu, or allergies? Learn how to tell the difference and when to see a provider. Take the Allergy Quiz or Find a Provider near you today. Understanding the Confusion Every fall, countless people wonder: Is it a cold, the flu, or allergies? Each…
Rising Ragweed Pollen: Why Fall Allergies in the U.S. Are Getting Worse
Every fall, ragweed pollen has long been a familiar culprit behind sneezing, congestion, and itchy eyes. But lately, it’s not just the symptoms that are changing—it’s the season itself. Rising ragweed pollen levels are making allergy season longer, more intense, and harder to escape. What…
Am I Suffering from Allergies? Or Something Else?
There is a wide range of variability from person to person when it comes to allergies. The unique circumstances of each person and their environment as well as what type of symptoms occur, how often they occur, and how troublesome they are all have significant meaning. Gathering this…
A Deep Dive into Summertime Allergies
As the warmth of summer graces us with its presence, many of us are eager to embrace outdoor activities and soak up the sun. However, along with the barbecues, beach days, and sunny strolls, comes an uninvited guest: allergies. For many people, summer is synonymous with sniffling, sneezing, itchy…
FSA/HSA Plans for Allergy Services
Environmental allergies are a common ailment that affects approximately 50 million Americans every year. Whether you suffer from year round or just seasonal allergies, you may be able to use your tax-free FSA/HSA funds to help you save money on education, allergy testing, and treatments. If you…
Oral Allergy Syndrome
Delicious, ripe, mouthwatering fruits and vegetables are more plentiful during these summer months. However, that that summer breeze may carry more than just excitement for the season. Some people with environmental allergies may notice that certain fruits, vegetables, or nuts give them distinct…
Summer Allergies
What do you look forward to in the summer months? I bet it isn't summer allergies! Whether you are planning to be the grill master or the ultimate host of the patio celebration, we have tips to help you prepare. Today, let’s discuss some common summer allergens you may encounter when enjoying the…
Eosinophilic Esophagitis (EoE)
Eosinophilic esophagitis (EoE) is a recognized diagnosis that produces symptoms related to dysfunction of the esophagus. In EoE, large amounts of white blood cells, specifically eosinophils, collect in the inner lining of the esophagus resulting in inflammation. Typically, the esophagus is free…
Allergies, Asthma, and Air Quality
As we move into the summer months, it is important to understand the connection between allergies, asthma, and air quality. While air pollution does not directly cause allergy or asthma, it can increase the risk of developing atopic disease. Air pollution can also trigger allergy or asthma symptoms…
Earth Day and Climate Change Effects
Earth Day is this Friday, April 22nd. Earth Day is truly a mainstay in American culture, created by Past-President Richard Nixon. This year the Earth Day theme is “Invest in Our Planet”. We are called upon to have “unstoppable courage to preserve and protect our health, our families, our…
Easter and Passover Allergy Concerns
The Easter and Passover holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, holidays like Easter and Passover can be challenging to navigate with traditional holiday foods containing hidden allergies, and the high…
Botanical Sexism: Does it impact allergy sufferers?
What is Botanical Sexism? Tom Ogren, horticulturist and allergy researcher, has done extensive research on ways to reduce pollen counts and pollen potency. His theory centers around the unbalanced planting of male vs female plants. This unbalance can impact pollen counts and the resulting…
Tree Pollen and Pollen Counts Explained
March is here, and so is Spring! Spring has officially started which brings longer days, refreshing rain showers, bright colorful flowers, and of course…tree pollen! The majority of trees typically produce tree pollen as early as January in the Southern United States. The Northern and Central areas…
St. Patrick’s Day, Green Beer, and Wheat Allergy
St. Patrick's Day is fast approaching! Are you wondering if your wheat allergy will get in the way? History of the Holiday In Ireland, the holiday was created as a way to honor the country's patron saint and a time to cut loose during the Catholic Lent season. Today, the holiday is honored in…
Shake off the winter blues!
Winter blues setting in? Dreaming of springtime? Well, the wait is almost over! March is a week away, and that means Spring is on its way! Longer days, long walks in the garden, and rain showers and rainbows are on the horizon. The meteorological calendar says spring begins March 1st, but the…
Six More Weeks of Winter
The first official Groundhog Day celebration took place on February 2, 1887, in Punxsutawney, Pennsylvania, and was the brainchild of local newspaper editor Clymer Freas. He sold a group of businessmen and groundhog hunters on the idea of gathering around the inaugural famous groundhog to see…
The BIG 9: Food Allergens
For the last 17 years, the official list of major food allergens, or “The Big 8” has consisted of milk, egg, fish, shellfish, peanut, tree nut, wheat, and soy. The Big 8 were part of legislation that was signed into law in 2004 requiring manufacturers to indicate on labels when a product was made…
Prepare for Spring Allergy Season
Spring is fast approaching, and if you are a seasonal allergy sufferer, you likely associate this time of year with chronic sneezing, sniffling, and coughing. Your immune system is armed and ready to defend against harmless pollens, sending histamine soaring in your body triggering sneezing, runny…
Contraindications for Immunotherapy
Allergies are not always clear cut and simple to understand. A person may assume that a certain food or substance is the cause of their allergy symptoms and relate it to allergies, or they may not see the complete picture. We know allergy testing is extremely beneficial in allowing a provider to…
2022 – New Year, New You!
Happy New Year, and welcome 2022! The start of a new year arrives for many with guilt-laden resolutions to improve things like personal health goals. Resolutions to improve health can seem overwhelming and cause anxiety if they are unrealistic in the end goal or timeframe. Allergy and asthma…
Helpful Hints for the Holidays
The holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, holidays like Christmas, Hanukkah, and Kwanza can be challenging. First, traditional holiday foods containing hidden allergies may be present. Also at risk is…
Eczema and Atopic Dermatitis
We have made it to the highly anticipated holiday season! We ate more than our share of turkey, taken down the last of the fall décor, have started trimming the tree, and are double down on the holiday gift lists. With winter weather upon us or in the near future, and personal care products a…
Dust Mite Allergy
Halloween may be over, but there are certain creepy creatures that diligently remain year-round and commonly trigger allergy and asthma symptoms. Dust mites are eight-legged relatives ticks and spiders, have no eyes, have translucent bodies, and are microscopic, or too small to see with the unaided…
Respiratory Care Week, October 24-30
As we settle into this final week of October and prepare for some frightful fun at the end of the week, let’s all take a big deep breath in before the end of the year holiday season is upon us! Speaking of that big deep breath, October is Healthy Lung Month and this week, October 24-30 is…
Football, Food, and Fall Allergies
Fall has arrived and so have shorter days, cooler weather, and football season! Unfortunately for some, football, food and fall allergies go hand in hand. This is especially true in the southern and western regions of the US where some weed allergens peak in the fall. The idea of sneezing and…
Flu, Allergies, Cold, or COVID?
With the approaching fall season, we typically witness flu and viral season quickly arrive as well. Simultaneously weed pollen, dust mite, and mold allergy sufferers are preparing for an intense time of year. This year however, the ongoing spread of COVID-19 and reputable variants adds an…
Ragweed and Fall Pollen Allergies
Back to school season is here! Shorter days, crisp, cool evenings, and beautiful fall foliage are on the horizon. This time also marks the onset of weed pollination and the resurgence of allergy symptoms that may have taken a vacation in the hot, dry July heat. The meteorological calendar says…
Back to School Action Plan for Allergies and Asthma
As the final days of summer break come to a close, families everywhere are preparing for children to return to school. Whether this is the first year a child is heading to school or the last, it is an exciting time for both children and parents. It can, however, also be a time of anxiety for a…
Stinging Insects & Allergic Reactions
As summer continues marching on, the calendar surely includes upcoming cook-outs, boating on the lake or just a few hours playing in the backyard. The warmer temperatures and longer days present increased opportunities for visits for not so welcome winged visitors. While stinging insects may only…
Summer Allergy Travel Tips
School is out, summer is in full swing, and it is prime time for summer vacations and traveling. Summer travel with environmental allergies, asthma, or food allergies may make planning a vacation seem like a daunting task. Not to worry! We can show how to keep summer allergy issues at bay during…
Grass Pollen Allergy: Making the Most of Summer
Summer is finally here! Longer days, days spent by the beach or the pool, and late nights catching fireflies are on the horizon. Allergies are usually associated with the spring or fall because pollen is most active during these times. However, summer allergies, especially to grass, are also…
Independence from Summer Allergies
The Fourth of July is only one week away and that likely means many are making or finalizing plans to be outside. Are you planning to be the grill master? How about the fireworks expert? Maybe you are the ultimate host of the celebration surrounded by family and friends enjoying fireworks, picnics,…
Easter with Allergies
The Easter and Passover holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, they can sometimes be challenging to navigate. Aside from the usual pollen and food allergies, brightly dyed eggs, household pets, and sweet…
Tips for Balancing Baseball and Allergies
Spring means longer days, warmer weather, and the beginnings of baseball! Unfortunately for some allergy sufferers, the start of the long-anticipated baseball season also means the time of year when allergens such as tree pollen are at an all-time high. Sneezing, wheezing, and itchy, watery eyes…
Tips for Traveling with Allergies
Summer is here, and for many families that means a much anticipated vacation! A time for overdue rest and relaxation, or maybe some quality time spent away with children and loved ones. While fun can be had at its best during this time, allergies can be at their worst, leaving sufferers to fear…
Tree Pollen Allergy
March is finally here, and that means so is Spring. Longer days, morning walks in the garden, rain showers and rainbows are excitedly on the horizon. However, if you have spring allergies you may be less excited about the season. Spring is typically defined as starting with the vernal equinox, and…
Skin Care Tips: Atopic Dermatitis & Eczema
From Amanda Hofmann, VP Clinical at United Allergy Services: Earlier this month, the famous groundhog, “Punxsutawney Phil”, saw his shadow and promised 6 more weeks of winter. This past week, Phil showed he was serious about that promise as winter storms swept across most of the US. This recent…
Are Hypoallergenic Pets a Real Thing?
Are you one of those people that think life without a furry friend is unimaginable? You aren’t alone. In fact, millions of dedicated pet owners even suffer through pet related allergy symptoms because life without a fur-baby isn't an option for them. In a growing trend, many steadfast animal lovers…
Valentine’s Day Allergy Offenders
Valentine's Day can be intimidating for allergy suffers. Far too frequently sweethearts visit the emergency room instead of their favorite restaurant or fill the day with sneezes instead of smooches. Avoiding the most common Valentine’s Day allergy offenders is possible, and here are some tips to…
‘Tis the season for Cedar Fever
In parts of Texas and surrounding areas, cedar allergies are one last health challenge in an already difficult year. 2020 has been one for the ages, headlined by the widespread impact of the COVID pandemic. While Americans and the rest of the world await a vaccine, there are other concerns that can…
Rural communities are big winners with value-added care
Rural communities in the United States are often underserved when it comes to access to healthcare. That's why National Rural Health Day is important; it provides a chance to shine light on the health challenges faced in rural America. Among those factors are distance, transportation, economics,…
How allergy care remains both accessible and essential during COVID
The COVID-19 pandemic continues to impact the entire country. Its effects have been uniquely felt in the healthcare industry, as providers reshape how they see patients and as Americans grow increasingly aware of their daily symptoms: is that lingering cough caused by a cold, the flu, or something…
David Boone on at-home allergy shots as potential long-term relief from “cedar fever”
Winter doesn't spell relief for all allergy sufferers -- especially in Texas and parts of other nearby states, where the colder weather signals the beginning of mountain cedar season. Cedar is one of the most severe allergens in areas where it is found. While locals will recognize the heavy,…
Press Release: Nation’s Largest Allergy Care Provider Celebrates 10 years
San Antonio-based United Allergy Services continues to serve and expand. SAN ANTONIO (October, 2019) – Since its founding in 2009, United Allergy Services has grown into the leading allergy diagnostic and immunotherapy services provider in the nation. Headquartered in San Antonio, the company has…
Back to School is the time to get tested before Fall Allergy Season begins
As Americans return to work and school from summer vacation, the fall allergy season will begin to impact many of the nearly 50 million allergy sufferers across the country. According to the Asthma and Allergy Foundation of America, Americans lost more than 6 million work and school days in 2018,…
MySA story highlights United Allergy Services’ role in the allergy space
In July, United Allergy Services was featured in a story on mySA.com. The first section of the article, titled "How immunotherapy is changing lives for people with allergies", looks at the allergy epidemic in America: "Allergies pose a genuine health risk beyond stuffy noses and itchy, watery eyes.…
2018 forecasts call for longer allergy seasons
American allergy sufferers have come to know what to expect throughout the year – oak in spring; grass over the late spring and early summer months; ragweed in late summer through autumn; cedar in fall through winter – as their fluctuating symptoms follow the changing of the seasons. Recent years,…
5 interesting cases of allergic cross-reactivity
Allergy sufferers cope with their sensitivities in a number of ways, from over-the-counter medication and immunotherapy treatment to simple avoidance. Yet, even if a person was to employ every known method of avoidance, it’s still possible he or she would still experience an allergic reaction at a…
Christmas Tree Syndrome
One of the early signs the holidays are coming is the sight of Christmas trees popping up in homes around your neighborhood. For some, that means pulling an artificial tree out of a box; for others, it means heading to the nearby tree farm to pick up a real one. Whichever you prefer, there are…
How to Minimize Dog Shedding
Dog shedding is a normal part of your dog’s life. You can’t stop shedding completely, but you can minimize it. What causes excessive shedding? A lack of nutrition (make sure your dog gets the right diet); dog shedding season (in the spring and later in the fall); health (some health problems such…
What It Actually Takes to Launch Allergy Services in 90 Days
Congratulations, you have made the decision to add a new service to improve your patients’ and your practice’s health—allergy testing and immunotherapy. Now what? Adding allergy testing and immunotherapy sounds complex, but it’s not with the right partner and mindset. Of course, there are the…
Is Your Practice Ready for Spring Allergy Season?
Every spring, there is a surge of patients experiencing symptoms such as congestion, sinus pressure, itchy eyes, cough, fatigue, and headaches. While these allergy symptoms are common, seasonal allergies affect more than 100 million Americans each year, making allergic rhinitis one of the most…
USP <797> Explained: What Physicians Need to Know When Preparing Allergen Immunotherapy In-Office
As regulatory standards evolve, many physician practices are asking an important question: How does USP <797> impact the way we prepare allergen immunotherapy (AIT) in our office? Whether you are currently mixing allergy extracts on site or considering adding immunotherapy services to your…
Fall Allergy Relief: How Provider Practices Can Lead the Way
As summer starts to give way to fall, and the first cool front arrives, many patients brace for seasonal allergies. While ragweed often steals the spotlight, fall allergy sufferers face a broader spectrum of triggers—from varied pollen sources to mold and dust mites. For many providers, this season…
Allergy Services for Primary Care Physicians: Expanding Access to Long-Term Allergy Relief
Allergies affect more than 100 million people each year. Yet despite their widespread impact, allergies often go untreated due to the scarcity of specialist care. That’s why United Allergy Services is focused on introducing allergy treatment and immunotherapy to primary care practices—the first and…
United Allergy Services Featured in Fujitsu Case Study
We are happy to share that United Allergy Services was recently featured in a Fujitsu case study highlighting how we achieve precise inventory tracking and process automation to enhance patient safety and efficiency. The case study explores how UAS leverages Fujitsu’s GLOVIA® OM solution, in…
Allergy Testing Kits & Immunotherapy from UAS: A Flexible Solution
Adding allergy care allows healthcare providers to address a common patient need and create a new income stream within the existing framework of their practice. However, we know that every medical practice has different requirements. For practitioners looking to integrate allergy testing and…
Pediatrics: How Early Allergy Testing & Treatment Can Benefit Young Patients
Allergies are a common yet often overlooked concern in pediatric care, affecting millions of children across the U.S. While allergy symptoms like sneezing, itchy eyes, and congestion may seem minor, untreated allergies can lead to more serious conditions, including asthma, chronic sinus infections,…
The Primary Care Practice Crisis: It’s Time to Play Offense
In an article published in Medical Economics, Brad J. Scoggins, FO, DAAP contends that it’s not enough for medical practices to counter adverse market forces by cutting costs and streamlining operations. He argues that practices must take steps to generate more revenue—specifically by offering…
Case Study: Adding Allergy Testing and Immunotherapy to Patient Care
A thriving practice delivering comprehensive patient services in-house, including family care, pediatrics, internal medicine, rheumatology, gynecology, and dietitian services, wanted to expand its offerings with on-site allergy testing and immunotherapy. The practice’s physician team strived to…
Maximizing Your Practice by Minimizing the Leakage
Does your medical practice have leaks? Is your growth hindered by “lost business” that negates the full impact of new patient growth? One of my favorite business expressions is from Roger Enrico, the former CEO of PepsiCo, who would say: “Growth is what matters.” It was one of the cornerstones that…
Why Offer Allergy Treatment for Children?
For providers passionate about providing care to the pediatric population, integrating fundamental allergy care into their practice can bring about significant benefits. Allergy screening, testing, and treatment fosters healthier lives and also enhances the overall quality of care that can be…
How Does UAS Partner with Providers?
How can healthcare providers balance the demands for more patient quality time and the financial requirements for a sustainable practice? Although it may seem counterintuitive to offer an additional service line, doing so can deliver higher revenue, additional clinical support, and meet rising…
Why Offer Allergy Care Services in Your Medical Practice?
More than 100 million Americans suffer from environmental, seasonal and perennial allergies, including ragweed, pollen, dust mites and animal dander. In addition, roughly 11% of adults and 7½% of children have a food allergy. Unfortunately, only a fraction seek treatment from a specialist,…
Ancillary Medical Services
In today’s world of declining insurance reimbursements and a multitude of competing options for patients to access care, vibrant, healthy practices are constantly seeking opportunities to grow. Growth can come from expanding your patient base as well as expanding your offerings by offering…
Am I Suffering from Allergies? Or Something Else?
There is a wide range of variability from person to person when it comes to allergies. The unique circumstances of each person and their environment as well as what type of symptoms occur, how often they occur, and how troublesome they are all have significant meaning. Gathering this…
A Deep Dive into Summertime Allergies
As the warmth of summer graces us with its presence, many of us are eager to embrace outdoor activities and soak up the sun. However, along with the barbecues, beach days, and sunny strolls, comes an uninvited guest: allergies. For many people, summer is synonymous with sniffling, sneezing, itchy…
FSA/HSA Plans for Allergy Services
Environmental allergies are a common ailment that affects approximately 50 million Americans every year. Whether you suffer from year round or just seasonal allergies, you may be able to use your tax-free FSA/HSA funds to help you save money on education, allergy testing, and treatments. If you…
Oral Allergy Syndrome
Delicious, ripe, mouthwatering fruits and vegetables are more plentiful during these summer months. However, that that summer breeze may carry more than just excitement for the season. Some people with environmental allergies may notice that certain fruits, vegetables, or nuts give them distinct…
Summer Allergies
What do you look forward to in the summer months? I bet it isn't summer allergies! Whether you are planning to be the grill master or the ultimate host of the patio celebration, we have tips to help you prepare. Today, let’s discuss some common summer allergens you may encounter when enjoying the…
Eosinophilic Esophagitis (EoE)
Eosinophilic esophagitis (EoE) is a recognized diagnosis that produces symptoms related to dysfunction of the esophagus. In EoE, large amounts of white blood cells, specifically eosinophils, collect in the inner lining of the esophagus resulting in inflammation. Typically, the esophagus is free…
Allergies, Asthma, and Air Quality
As we move into the summer months, it is important to understand the connection between allergies, asthma, and air quality. While air pollution does not directly cause allergy or asthma, it can increase the risk of developing atopic disease. Air pollution can also trigger allergy or asthma symptoms…
Earth Day and Climate Change Effects
Earth Day is this Friday, April 22nd. Earth Day is truly a mainstay in American culture, created by Past-President Richard Nixon. This year the Earth Day theme is “Invest in Our Planet”. We are called upon to have “unstoppable courage to preserve and protect our health, our families, our…
Easter and Passover Allergy Concerns
The Easter and Passover holidays are here! Holidays mean family centered fun, festive meals, and usually sweet treats to enjoy. For allergy suffers, however, holidays like Easter and Passover can be challenging to navigate with traditional holiday foods containing hidden allergies, and the high…
Botanical Sexism: Does it impact allergy sufferers?
What is Botanical Sexism? Tom Ogren, horticulturist and allergy researcher, has done extensive research on ways to reduce pollen counts and pollen potency. His theory centers around the unbalanced planting of male vs female plants. This unbalance can impact pollen counts and the resulting…
Tree Pollen and Pollen Counts Explained
March is here, and so is Spring! Spring has officially started which brings longer days, refreshing rain showers, bright colorful flowers, and of course…tree pollen! The majority of trees typically produce tree pollen as early as January in the Southern United States. The Northern and Central areas…
St. Patrick’s Day, Green Beer, and Wheat Allergy
St. Patrick's Day is fast approaching! Are you wondering if your wheat allergy will get in the way? History of the Holiday In Ireland, the holiday was created as a way to honor the country's patron saint and a time to cut loose during the Catholic Lent season. Today, the holiday is honored in…
Shake off the winter blues!
Winter blues setting in? Dreaming of springtime? Well, the wait is almost over! March is a week away, and that means Spring is on its way! Longer days, long walks in the garden, and rain showers and rainbows are on the horizon. The meteorological calendar says spring begins March 1st, but the…
Six More Weeks of Winter
The first official Groundhog Day celebration took place on February 2, 1887, in Punxsutawney, Pennsylvania, and was the brainchild of local newspaper editor Clymer Freas. He sold a group of businessmen and groundhog hunters on the idea of gathering around the inaugural famous groundhog to see…
The BIG 9: Food Allergens
For the last 17 years, the official list of major food allergens, or “The Big 8” has consisted of milk, egg, fish, shellfish, peanut, tree nut, wheat, and soy. The Big 8 were part of legislation that was signed into law in 2004 requiring manufacturers to indicate on labels when a product was made…
Prepare for Spring Allergy Season
Spring is fast approaching, and if you are a seasonal allergy sufferer, you likely associate this time of year with chronic sneezing, sniffling, and coughing. Your immune system is armed and ready to defend against harmless pollens, sending histamine soaring in your body triggering sneezing, runny…
Contraindications for Immunotherapy
Allergies are not always clear cut and simple to understand. A person may assume that a certain food or substance is the cause of their allergy symptoms and relate it to allergies, or they may not see the complete picture. We know allergy testing is extremely beneficial in allowing a provider to…
2022 – New Year, New You!
Happy New Year, and welcome 2022! The start of a new year arrives for many with guilt-laden resolutions to improve things like personal health goals. Resolutions to improve health can seem overwhelming and cause anxiety if they are unrealistic in the end goal or timeframe. Allergy and asthma…
Respiratory Care Week, October 24-30
As we settle into this final week of October and prepare for some frightful fun at the end of the week, let’s all take a big deep breath in before the end of the year holiday season is upon us! Speaking of that big deep breath, October is Healthy Lung Month and this week, October 24-30 is…
Football, Food, and Fall Allergies
Fall has arrived and so have shorter days, cooler weather, and football season! Unfortunately for some, football, food and fall allergies go hand in hand. This is especially true in the southern and western regions of the US where some weed allergens peak in the fall. The idea of sneezing and…
Ragweed and Fall Pollen Allergies
Back to school season is here! Shorter days, crisp, cool evenings, and beautiful fall foliage are on the horizon. This time also marks the onset of weed pollination and the resurgence of allergy symptoms that may have taken a vacation in the hot, dry July heat. The meteorological calendar says…
Back to School Action Plan for Allergies and Asthma
As the final days of summer break come to a close, families everywhere are preparing for children to return to school. Whether this is the first year a child is heading to school or the last, it is an exciting time for both children and parents. It can, however, also be a time of anxiety for a…
Summer Allergy Travel Tips
School is out, summer is in full swing, and it is prime time for summer vacations and traveling. Summer travel with environmental allergies, asthma, or food allergies may make planning a vacation seem like a daunting task. Not to worry! We can show how to keep summer allergy issues at bay during…
Grass Pollen Allergy: Making the Most of Summer
Summer is finally here! Longer days, days spent by the beach or the pool, and late nights catching fireflies are on the horizon. Allergies are usually associated with the spring or fall because pollen is most active during these times. However, summer allergies, especially to grass, are also…
Independence from Summer Allergies
The Fourth of July is only one week away and that likely means many are making or finalizing plans to be outside. Are you planning to be the grill master? How about the fireworks expert? Maybe you are the ultimate host of the celebration surrounded by family and friends enjoying fireworks, picnics,…
5 ways to boost your healthcare practice in 2021
Every new year offers exciting possibilities, but it’s fair to assume that 2021 bears more anticipation than usual. At the center of the optimism is the arrival and distribution of the COVID-19 vaccine–and the return to normalcy it will bring to communities around the country. For…
‘Tis the season for Cedar Fever
In parts of Texas and surrounding areas, cedar allergies are one last health challenge in an already difficult year. 2020 has been one for the ages, headlined by the widespread impact of the COVID pandemic. While Americans and the rest of the world await a vaccine, there are other concerns that can…
Rural communities are big winners with value-added care
Rural communities in the United States are often underserved when it comes to access to healthcare. That's why National Rural Health Day is important; it provides a chance to shine light on the health challenges faced in rural America. Among those factors are distance, transportation, economics,…
How allergy care remains both accessible and essential during COVID
The COVID-19 pandemic continues to impact the entire country. Its effects have been uniquely felt in the healthcare industry, as providers reshape how they see patients and as Americans grow increasingly aware of their daily symptoms: is that lingering cough caused by a cold, the flu, or something…
David Boone on at-home allergy shots as potential long-term relief from “cedar fever”
Winter doesn't spell relief for all allergy sufferers -- especially in Texas and parts of other nearby states, where the colder weather signals the beginning of mountain cedar season. Cedar is one of the most severe allergens in areas where it is found. While locals will recognize the heavy,…
David Boone speaks with MD Magazine about bridging the gap in allergy care
What can primary care providers and companies like United Allergy Services do to address the allergy epidemic in this country? UAS's Chief Executive Officer, David Boone, recently discussed that and more in an interview with MD Magazine. "It's a lifestyle issue, it's a productivity issue, it's a…
United Allergy Services’ Hugh Spires on providing counsel in a time of growth and innovation
United Allergy Services' General Counsel and Vice President, Hugh Spires, recently spoke with Vanguard Law Magazine about the work we and the providers we work with are doing to improve lives, as well as the role he's played in helping UAS push new boundaries in allergy care. You can currently read…
United Allergy Services C.E.O. talks about redefining the allergy care industry
United Allergy Services' Chief Executive Officer David Boone recently wrote an article for D CEO Healthcare about the vital role that primary care providers can play in addressing the nationwide gap in allergy care. Boone addresses the limitations in how the healthcare industry has traditionally…
Press Release: Nation’s Largest Allergy Care Provider Celebrates 10 years
San Antonio-based United Allergy Services continues to serve and expand. SAN ANTONIO (October, 2019) – Since its founding in 2009, United Allergy Services has grown into the leading allergy diagnostic and immunotherapy services provider in the nation. Headquartered in San Antonio, the company has…
United Allergy Services names new Vice President of Strategic Growth
United Allergy Services has announced the hiring of David Cheetham as the organization’s Vice President of Strategic Growth. Cheetham will drive the organization’s expansion efforts to provide allergy diagnostics and long-term relief in a growing number of markets moving forward. A leader with…
Rural communities are big winners with value-added care
Rural communities in the United States are often underserved when it comes to access to healthcare. That's why National Rural Health Day is important; it provides a chance to shine light on the health challenges faced in rural America. Among those factors are distance, transportation, economics,…
How allergy care remains both accessible and essential during COVID
The COVID-19 pandemic continues to impact the entire country. Its effects have been uniquely felt in the healthcare industry, as providers reshape how they see patients and as Americans grow increasingly aware of their daily symptoms: is that lingering cough caused by a cold, the flu, or something…
David Boone on at-home allergy shots as potential long-term relief from “cedar fever”
Winter doesn't spell relief for all allergy sufferers -- especially in Texas and parts of other nearby states, where the colder weather signals the beginning of mountain cedar season. Cedar is one of the most severe allergens in areas where it is found. While locals will recognize the heavy,…
David Boone speaks with MD Magazine about bridging the gap in allergy care
What can primary care providers and companies like United Allergy Services do to address the allergy epidemic in this country? UAS's Chief Executive Officer, David Boone, recently discussed that and more in an interview with MD Magazine. "It's a lifestyle issue, it's a productivity issue, it's a…
United Allergy Services’ Hugh Spires on providing counsel in a time of growth and innovation
United Allergy Services' General Counsel and Vice President, Hugh Spires, recently spoke with Vanguard Law Magazine about the work we and the providers we work with are doing to improve lives, as well as the role he's played in helping UAS push new boundaries in allergy care. You can currently read…
United Allergy Services C.E.O. talks about redefining the allergy care industry
United Allergy Services' Chief Executive Officer David Boone recently wrote an article for D CEO Healthcare about the vital role that primary care providers can play in addressing the nationwide gap in allergy care. Boone addresses the limitations in how the healthcare industry has traditionally…
Press Release: Nation’s Largest Allergy Care Provider Celebrates 10 years
San Antonio-based United Allergy Services continues to serve and expand. SAN ANTONIO (October, 2019) – Since its founding in 2009, United Allergy Services has grown into the leading allergy diagnostic and immunotherapy services provider in the nation. Headquartered in San Antonio, the company has…
United Allergy Services names new Vice President of Strategic Growth
United Allergy Services has announced the hiring of David Cheetham as the organization’s Vice President of Strategic Growth. Cheetham will drive the organization’s expansion efforts to provide allergy diagnostics and long-term relief in a growing number of markets moving forward. A leader with…
Back to School is the time to get tested before Fall Allergy Season begins
As Americans return to work and school from summer vacation, the fall allergy season will begin to impact many of the nearly 50 million allergy sufferers across the country. According to the Asthma and Allergy Foundation of America, Americans lost more than 6 million work and school days in 2018,…
MySA story highlights United Allergy Services’ role in the allergy space
In July, United Allergy Services was featured in a story on mySA.com. The first section of the article, titled "How immunotherapy is changing lives for people with allergies", looks at the allergy epidemic in America: "Allergies pose a genuine health risk beyond stuffy noses and itchy, watery eyes.…
United Allergy Services Launches Mobile Healthcare App to Encourage Patient Medication Adherence
‘myAllergyPal®’ Allows Patients Undergoing Immunotherapy Treatment to Track Symptoms, Medication and Medical Appointments SAN ANTONIO, March 6, 2014 – United Allergy Services (UAS), a leading healthcare services company that enables family physicians, pediatricians and health systems to deliver…
UAS WAO Abstract Published Online
Congratulations to Frederick M. Schaffer, M.D., CMO; Larry Garner, allergy consultant; and Andrew Naples, clinical research coordinator; on the recent publication of The Safety of the United Allergy Services Immunotherapy Protocol. The abstract was published online in a supplement to the World…
United Allergy Services streamlines HR and recruitment: Salesforce.com-integrated solution eases document management for UAS
Founded in 2009, United Allergy Services (UAS) provides effective allergy testing and immunotherapy to the healthcare systems and professionals that treat patients with seasonal and perennial allergies. Employing over 800 people, the service line features an in-office Allergy Centre, staffing and…
Fairsail Streamlines Human Resources and Recruitment Processes for United Allergy Services
Reading, UK 1 Oct 2013 – Fairsail, the leader in Global Workforce Collaboration, today announced United Allergy Services (UAS), a leading healthcare services company empowering doctor and health systems to deliver safe and effective allergy testing and immunotherapy services, has selected it to…
AccessMD Urgent Care Teams with United Allergy Services to Expand Allergy Care Offerings
COLUMBUS, Ohio, Sept. 4, 2013/ -- AccessMD Urgent Care (which also operates as Hometown Urgent Care) today announced that it has partnered with United Allergy Services® (UAS), a leading healthcare services company empowering family physicians and health systems to deliver safe and effective allergy…
Kenneth Burdick Named Executive Vice Chairman of United Allergy Services Board of Directors
SAN ANTONIO, Texas – August 28, 2013 – United Allergy Services(UAS)™, the leading healthcare services company empowering physicians and health systems to deliver safe and effective allergy testing and customized immunotherapy services, today announced that Kenneth Burdick has accepted the role of…
United Allergy gets big booster shot from private-equity firm Serent Capital
Private-equity firm Serent Capital has acquired an ownership stake in United Allergy Services (UAS). That deal is expected to give San Antonio-based UAS more financial muscle, a greater diversity of operational expertise and an ability to pursue more growth opportunities nationally.
United Allergy Services Joins the American Academy of Family Physicians Foundation Corporate Partner Program
San Antonio, Texas — February 17, 2012 — United Allergy Services (UAS)™, the leading health care services company empowering physicians and health systems to deliver safe and effective allergy testing and customized immunotherapy services to patients, has joined the American Academy of Family…
United Allergy Services Announces Company Rebrand
San Antonio, TX— February 14, 2012— United Allergy Services (UAS)™, formerly known as United Allergy Labs™, today announced the company’s new name to better reflect its service role in the delivery of allergy testing and immunotherapy. United Allergy Services is the principal healthcare services…
LAFP Welcomes New Partner – United Allergy Labs
United Allergy Labs (UAL) attended the Annual Assembly & Exhibition for the first time in August. UAL specializes in providing fully-staffed and operational allergy services inside physicians’ offices. “We enjoyed meeting the LAFP physicians at the trade show and telling them about our allergy…