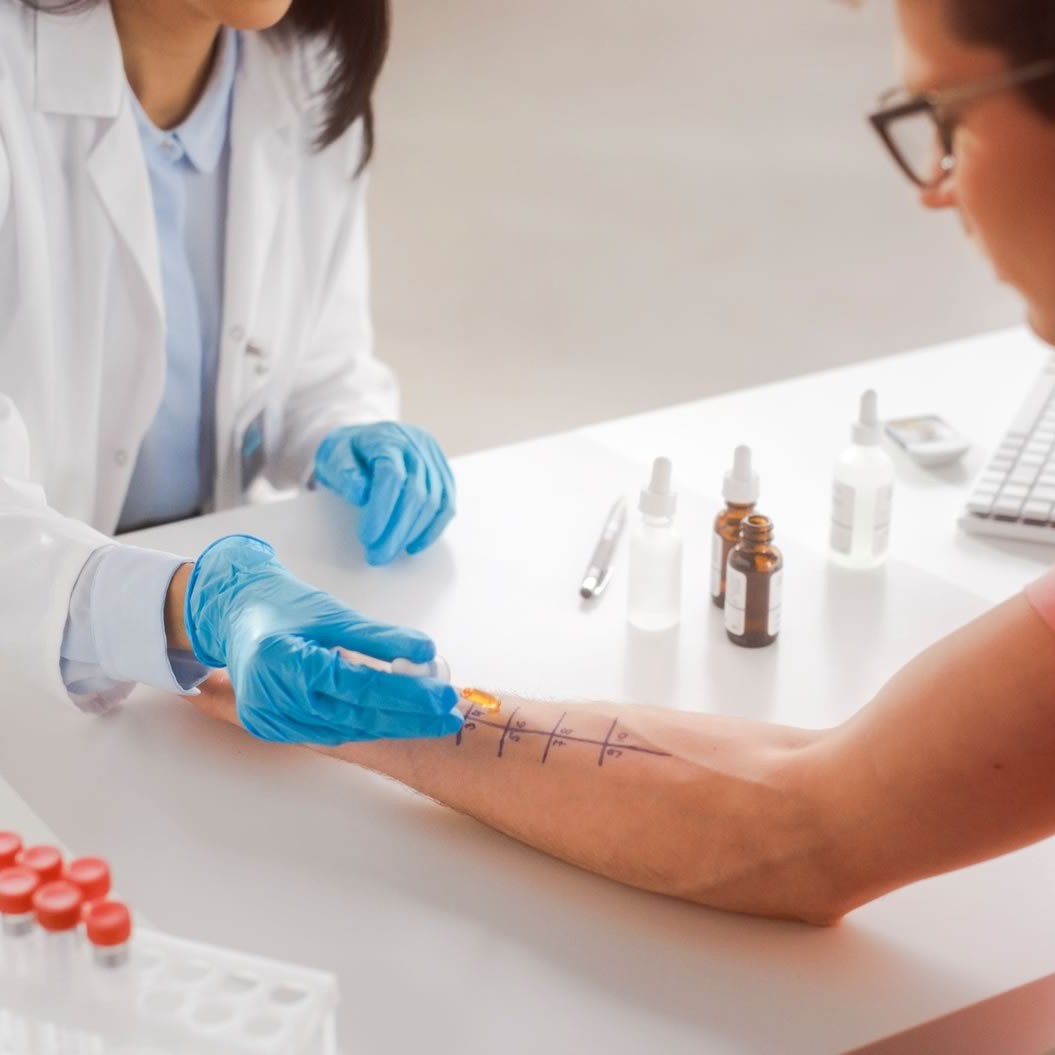
Allergies are not always clear cut and simple to understand. A person may assume that a certain food or substance is the cause of their allergy symptoms and relate it to allergies, or they may not see the complete picture. We know allergy testing is extremely beneficial in allowing a provider to determine precisely what is or is not causing troublesome symptoms. Accurate diagnosis of the allergy, along with insights into any current medications that have failed to improve or control symptoms, avoidance measures taken, and impact on daily life enables your provider to determine the best treatment program which often includes immunotherapy.
When a provider is considering allergy testing and immunotherapy, it is important to take into consideration potential contraindications that may warrant a different approach including potentially refraining to utilize United Allergy protocol in a particular patient. A contraindication in our instance is a particular condition which makes allergy testing or allergen immunotherapy potentially inadvisable. A contraindication may be absolute meaning that is any situation that this condition is present it is definitely not advised allergy testing or immunotherapy is utilized. The majority of contraindications applicable to allergy testing and immunotherapy, however, are relative. A relative contraindication means a certain condition can drive concern and could increase risks making it possibly inadvisable. Risk versus benefit assessment needs to take place.
Specific Contraindications
Patients that present with one or more of the following contraindications should be screened thoroughly by the provider and the benefits for testing and treating patients with immunotherapy must be weighed against the risks associated. This important assessment and determination on how to proceed will always rest with the ordering provider directly supervising the care of the patient.
- Beta Blockers: We highly recommend providers that have patients on beta-blockers consider switching them to another medication if appropriate prior to initiating immunotherapy. A beta-blocker may mask cardiac signs or symptoms related to anaphylaxis. Also, if a patient has an adverse event, they may not respond to the epinephrine needed to counteract the life-threatening reaction. There is currently limited data available to support holding beta blockers for a short time period such as 24 hours prior to an allergy test or immunotherapy dose to increase a patient’s safety.
- ACE Inhibitors: ACE inhibitors have been another cardiac medication thought to pose a risk if utilized with immunotherapy. ACE Inhibitors are considered due to their mechanism of action although whether they pose a significant risk as always been a major topic in academia. During an adverse reaction, it is thought that an ACE inhibitor can block the endogenous compensatory response manifested by the increased secretion of angiotensin-converting enzymes and prevent the destruction of kinins produced during the anaphylactic episode. The evidence regarding a true increased risk has not been clearly proven with environmental allergen immunotherapy and so is not currently included on our list of potential contraindications. Currently, data supports increased risk in venom allergen immunotherapy which is not offered under UAS protocol.
- Cardiac conditions: Patients with historic and current cardiac issues such as congestive heart failure, myocardial infarction, labile arrhythmias, uncontrolled hypertension, or other significant cardiac problems could be negatively challenged clinically if they experience anaphylaxis due to allergy testing or immunotherapy. Furthermore, many of these patients may not successfully tolerate the consequences of epinephrine injections if required to treat anaphylaxis.
- Previous history of anaphylaxis to aero allergens: Patients that have a history of previous reactions are much more likely to have a repeat reaction, oftentimes more severe than the initial reaction.
- Pregnancy: Pregnant patients must remain at the same concentration level of immunotherapy throughout the pregnancy and should not increase the dosage volume or concentration. This is because repeating the same positively tolerated dose, protects the expectant mother and developing fetus from potential harmful effects of epinephrine should a significant systemic reaction occur. It is beneficial for patients that become pregnant or plan to become pregnant at prior to testing, or at low dosage/concentration, delay allergy testing and immunotherapy until the pregnancy has concluded.
- HIV positive/ AIDS patients: AIDS or AIDS associated disorders are absolute contraindications to immunotherapy, however HIV+ status only is not always contraindicated according to literature. UAS currently recommends providers with patients with a positive HIV + status consider seeking an alternative protocol with an opportunity for closer and more consistent in office monitoring. However, despite this advisement, it is important to share there is no current absolute contraindication for a patient with a positive HIV status to begin allergen immunotherapy. There also are no large, controlled studies that can provide validity to the risks or to the benefits of allergen immunotherapy in HIV positive patients. There have been citations in recent literature to demonstrate both a negative response to initiation of immunotherapy (in which T-cell proliferation and RNA viral load increase occurred) and a positive response (a 3.5-year course of immunotherapy reduced symptoms and medication use, as well as provided well controlled symptoms 3 years port IT, without significant impact to HIV disease). Each patient must be closely assessed on an individual basis.
- Immunocompromised patients/ chemotherapy patients (including AIDS patients as mentioned above): Immunocompromised patients have not been shown in the literature to receive benefit from immunotherapy. Immunotherapy works by changing the T-cell repertoire. In immunocompromised patients T-cells are often altered. Thus, patients with an immunocompromised state are not recommended as candidates for immunotherapy.
- Patients with autoimmune diseases or utilizing immunosuppressant medications: As quoted from the AAAAI “Although concern about the safety of allergen immunotherapy in patients with autoimmune disorders has been raised in the past, there is no substantive evidence that such treatment is harmful in patients with these diseases.” Due to the variation in these different disease states and individual patient situations, it is recommended the benefits and risks are assessed on an individual basis. When a patient is utilizing an immunosuppressant medication there are theoretical concerns that immunotherapy’s benefit could be lessened, however there is no overarching body of evidence in literature that provides clear evidence of this regard. The best guidance I can provide for the ordering provider is to have full transparency with the patient regarding the theoretical concern of decreased efficacy of IT and considering holding immunotherapy during active exacerbations of autoimmune diseases.
- Uncontrolled asthma/severe asthma/severe COPD: The group of patients with the highest risk of severe reactions to allergy testing or allergen immunotherapy are asthmatics, particularly those that have uncontrolled or severe asthma. This can apply to anyone with impairment, obstruction, or restriction of their airways. To protect against a negative outcome of a severe systemic reaction it is strongly recommended providers do not test, initiate immunotherapy, or continue immunotherapy while a patient is in a compromised respiratory state.
- Eosinophilic Esophagitis (EoE) or Gastroenteritis: This is a concern that applies to sublingual immunotherapy ONLY and does not pertain to subcutaneous immunotherapy. In sublingual immunotherapy, the allergen is swallowed and has direct contact with the esophagus. Swallowed food, and an allergic response to the food or allergen is presumed to be important in the development or worsening of EoE. Therefore, it is thought that exposure of an aeroallergen with the esophagus can produce the same effects. Package inserts for the FDA approved SLIT tablets indicate that eosinophilic esophagitis is a contraindication for use.
- Inability to communicate: Patients undergoing allergy testing or allergen immunotherapy need to possess the ability to both mentally and physically participate in their diagnostic and/or treatment plan. The ability to clearly express and communicate active symptoms is crucial should an adverse reaction occur. Patients also need to possess the mental ability to understand the procedure or treatment ordered for them, be cooperative during the process, and understand the importance of their compliance.
Safety & Efficacy
United Allergy Services believes in appropriate patient selection (taking into consideration relative and absolute contraindications), doses building in a low, slow deliberate manner, and treatment in compliance with the relevant standards of practice guidelines. The proven safety results and efficacy of the self-administered subcutaneous immunotherapy protocol developed by United Allergy Services is based on a pre-selection of low-risk patients. If there are additional questions or any additional information requested, please contact the Clinical Support Team. We are here to support providers and provide guidance as they provide excellent allergy care to their patients.
Amanda Hofmann, MPAS, PA-C, is a graduate of Duquesne University, in Pittsburgh, Pennsylvania. After spending eight years in clinical practice, she joined United Allergy Services as the vice president of clinical. Amanda is also the past president of the Association of PAs in Allergy, Asthma, and Immunology.
United Allergy Services is also on Facebook, LinkedIn, or Twitter. See other interesting and related articles on the UAS Blog.
You may also be interested in . . .
Allergy Services for Primary Care Physicians: Expanding Access to Long-Term Allergy Relief
Allergies affect more than 100 million people each year. Yet despite their widespread impact, allergies often go untreated due to the scarcity of…
Allergy Testing Kits & Immunotherapy from UAS: A Flexible Solution
Adding allergy care allows healthcare providers to address a common patient need and create a new income stream within the existing framework of their…
Case Study: Adding Allergy Testing and Immunotherapy to Patient Care
A thriving practice delivering comprehensive patient services in-house, including family care, pediatrics, internal medicine, rheumatology, gynecology,…